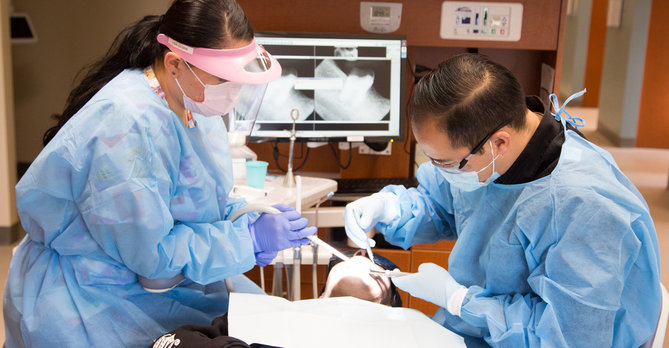
Poor access to dental services and growing racial/ethnic disparities in oral health is a growing concern in the safety net.
Prior to the ACA, 44 million Americans had no health insurance, but 100 million were without dental coverage. Most uninsured and underserved populations rely on Medicaid for dental coverage, yet many states are cutting budgets and eliminating dental benefits. Models of primary care-oral health integration require addressing financing and delivery barriers, developing service linkages and community resources, and strengthening the safety net itself through capacity building. Federal law and regulations related to the Early Periodic, Screening, Diagnosis and Treatment (EPSDT) program require that states provide medically necessary dental services for children, but state policies for adult dental coverage vary greatly — some states do not cover dental services at all, some limit coverage to specific adult populations, such as pregnant women, and others limit coverage to conditions associated with trauma or disease. Nationally 24% of health center services provided are dental services (14-20% per year in California), and over 70% of health centers provided oral health services on site as of 2005. Given that many health centers have co-located dental services, coordination seems to be more of the focus for dental integration.
A 2008 California Healthcare Foundation study reported a myriad of barriers that CHCs in California face in expanding dental services. These barriers fell into four main categories: start up and operating costs; payer mix, reimbursement and uncompensated care; recruitment, retention and training of staff; and leadership and management factors such as quality measures and efficiency. In 2011, an Institute of Medicine Report, “Improving Access to Oral Health Care for Vulnerable and Underserved Populations,” further underscored the health disparities that exist in oral health, and made multiple recommendations for adoption which include: working with states to increase Medicaid and Children’s Health Insurance Program reimbursement rates and address scope of practice barriers; providing non-dental healthcare professionals with training and skills to perform oral screenings and preventive services; and training dental professionals to care for complex, underserved patients in community-based settings.
Preventive dental care treatment reduces the incidence of oral disease and is a cost-effective proposition for Medicaid and other insurers, as it leads to reduction in costly emergency department visits.
In the full report, we describe a number of strategies to increase access to oral health services for all patients. Many of the innovations described in this section overlap multiple domains.