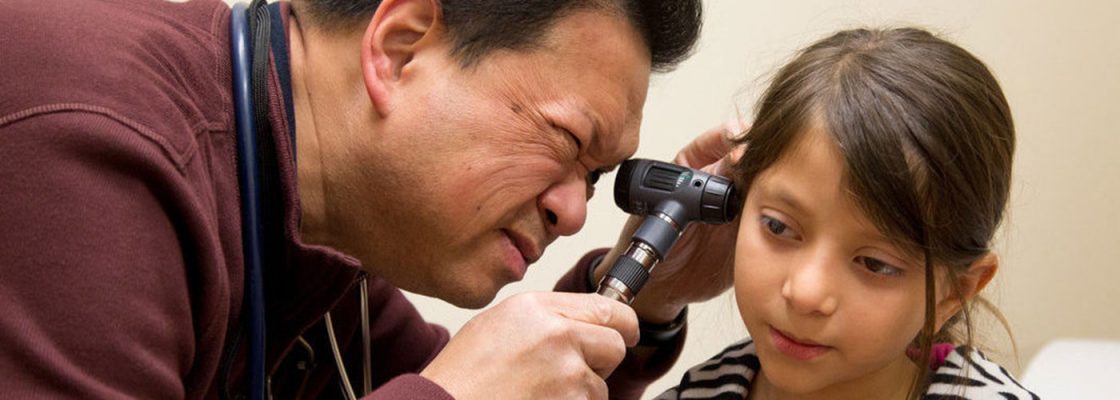
Nearly half of adults with health issues report problems with the coordination of their care in the United States. As Community Health Centers (CHCs) and other safety net settings transform into Patient-Centered Medical Homes, their role in the larger medical neighborhood will become pronounced. However, challenges with care coordination are magnified in the safety net setting and continue to be increasingly complex.
In 2014, the UCSF Center for Excellence in Primary Care, with funding from the Blue Shield of California Foundation, completed a comprehensive literature review outlining strategies CHCs use to integrate into the medical neighborhood in the domains of primary care-specialty care, primary care-diagnostic imaging, primary care-pharmacy, primary care-oral health and primary care-hospital care. A conceptual model which was used to classify innovations and strategies for integration can be found in the full report here.
The UCSF Center for Excellence in Primary Care has partnered with the Center for Care Innovations to develop this online resource center. The purpose of this Care Integration site is to disseminate resources, build connections and provide a platform for inter-agency learning and collaboration as Community Health Centers tackle care integration challenges across the country. Assess your practice’s care coordination strengths and opportunities using full or domain-specific self-assessment tools, or find out what other health centers are doing through case studies and webinars.
Focus Areas
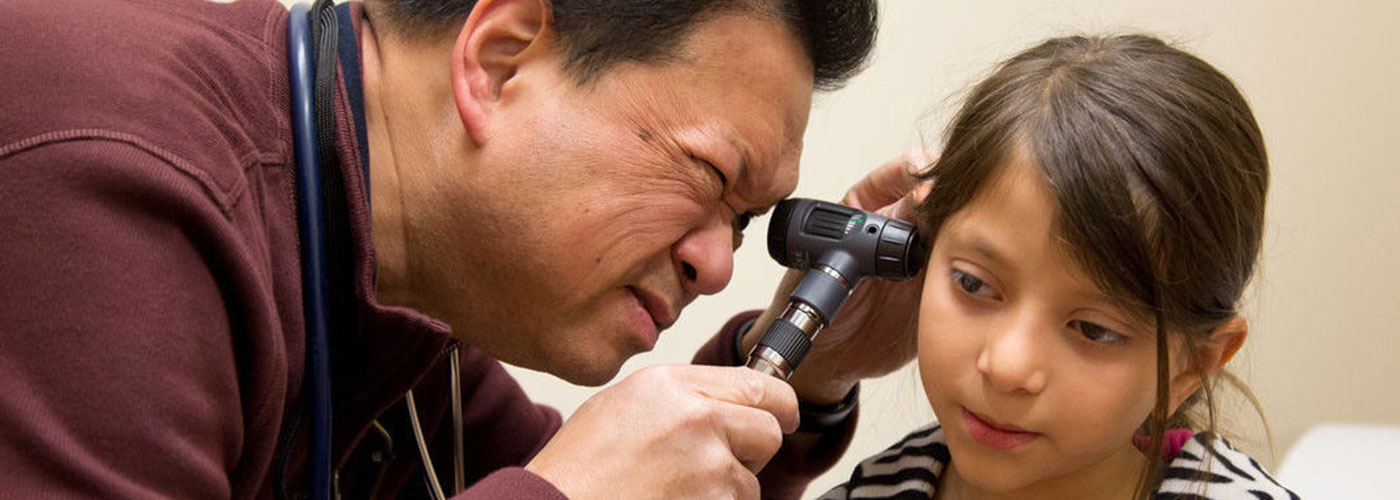
Integrating Primary Care and Specialty Care
One in four primary care visits at community health centers results in a referral to a specialist, from an endocrinologist to an oncologist, a dietician to an ophthalmologist. However long wait times and poor coordination can make it difficult for these patients to access the speciality care they need.
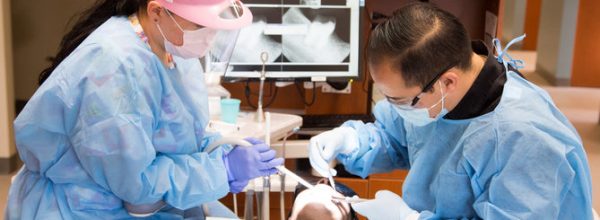
Integrating Primary Care and Oral Health
Poor access to dental services and growing racial/ethnic disparities in oral health is a growing concern in the safety net. Integrating oral health into community health centers is a powerful way to improve the lives and health of vulnerable patients.
Integrating Primary Care and Diagnostic Imaging
X-rays, mammography, ultrasound, CT scans and MRIs—imaging technologies offer a diagnostic tool vital to high-quality primary care. However vulnerable and uninsured patients may have difficulty accessing these high-cost services.
Integrating Primary Care and Pharmacy Care
Prescribing medications is a big part of primary care, but studies show about a quarter of first-time prescriptions are never filled, and an additional 30-40% of chronic disease medications are discontinued, taken incorrectly, or not picked up on time by patients.
Integrating Primary Care and Hospital Care
When patients have acute episodes, the hospitals that admit them too often lack the medical and social history that primary care providers know well. When patients are discharged from the hospital, their primary providers are too often left out of the loop on their care plan.