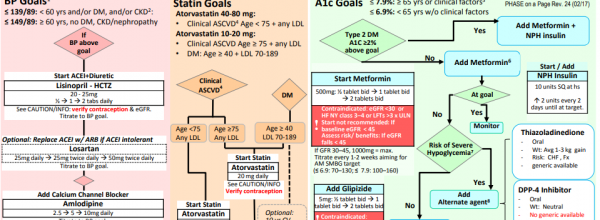
Four years ago, Kaiser Permanente introduced LifeLong Medical Care to its award-winning population health management program to care for people most at risk for heart attacks and strokes. It’s called PHASE, or Preventing Heart Attacks and Strokes Everyday.
Douglas Frey, a family nurse practitioner at LifeLong’s Downtown Oakland Health Center, recently walked us through how this resource helped improve hypertension control for the community’s underserved patients.
Rallying the Team
When a Kaiser Permanente doctor came to LifeLong’s all-provider meeting to discuss PHASE, it was an “ah-ha” moment for Douglas. He asked the clinical care associate if they could go into the electronic health record and pull data on his patients whose blood pressure was over 140/90 at their last visit. Out came a list of around 150 patients.
Next, Douglas met with the clinic manager to start an outreach program for this group of patients. Together, they came up with the idea of taking two of his regular 15-minute visits every day and turning them into a set of five 3-minute visits that focused on blood pressure checks.
Douglas then launched a brainstorm with his team about how to rollout these “little blood pressure check only visits.” Over lunch with a clinical care associate, community health worker, medical assistant, and nurse, Douglas described Kaiser’s algorithm, the different medications, and when to check labs. Where could they do these visits? Ultimately, they decided to carry out these visits at the blood pressure check station.
Testing Out Mini Appointments
This is how Douglas’s new mini appointments worked:
- A medical assistant would knock on the door of an exam room.
- Douglas would excuse himself to address a patient’s blood pressure at the vitals station.
- Then he would return to the exam room in under 3 minutes.
As opposed to blood pressure patients feeling like, “Oh he’s just in-and-out and barely spent time with me,” they liked that Douglas was coming out to visit them. The fact that he was stepping away from his exam room patient made that visit feel more critical.
Douglas said, “I think that’s an important kind of emotional part of a visit. They understood the importance of it because I was coming out to the station to talk with them about it.”
‘Low Hanging Fruit’
When PHASE first started at the clinic, blood pressure control hovered around 55 percent controlled.
To improve that number, LifeLong decided to start targeting patients at both ends of the spectrum — healthy patients who most likely needed a recheck and patients who were most at risk.
What Douglas called the “low hanging fruit” were patients who’d been just out of range, for example, someone with a blood pressure level of 142/68. After getting an accurate blood pressure check, the clinic found most of these patients’ blood pressure was controlled. Right off the bat, that boosted the clinic’s control rate by 10 percent to 65 percent controlled.
“You know, it’s someone who’s probably totally healthy but we just didn’t recheck because it was not on anyone’s radar,” Douglas said.
The team also discovered that people were confused about their medications because about 10 percent of the clinic’s uncontrolled patients couldn’t read. Rather than referencing the instructions, they’d be talking to staff about the “little orange pill” and “the green one.” So, the nurse started meeting with these patients every week to organize their medicines for them. She kept doing that until their blood pressure was controlled, then had their medications bubble-packed for them.
Helping Andre
Others had trouble with compliance. When it came to targeting high-risk patients, a patient named “Andre” changed Douglas’s entire perspective:
The clinic learned that it is so important to take the extra time to make sure patients understand hypertension. Be a stickler. Don’t let a patient go who is above controlled because they “just didn’t take their meds that day” or “hurried to the appointment.” By letting them off the hook, it allows them to think that perhaps blood pressure isn’t that important.
In a matter of months, so few patients were uncontrolled that Douglas could just call them on the phone. (Even a number of patients experiencing homelessness have cell phones.)
This work whittled down the number of really uncontrolled patients. However, heartbreakingly, they started dropping off the clinic’s roster because they either passed away or had to move to other care facilities because of heart attacks and strokes.
The Importance of Buy-In
One of the first challenges to implementing PHASE was ensuring that the staff was checking blood pressure correctly — resting, feet on the ground, arm at heart height. If it’s too elevated, you need to recheck. You need the right size cuff because size also makes a real difference. Douglas had to demonstrate to the staff the importance of doing this right, and they listened.
Once Douglas made it through his panel — somewhere between 700 and 900 patients — the clinic introduced Douglas’s PHASE idea to three other clinicians. Gradually, as more staff understood what the “blood pressure check only visits” were for, they were able to allow other staffers to start scheduling them.
One physician initially held out — but Douglas eventually won her over:
It took creating a culture around PHASE, so those numbers on a page are more than just stats. It was about creating an environment where no patient left the clinic without a follow-up plan and recheck. All this work meant that it didn’t matter which provider a patient saw because everyone knew the next PHASE step.
Soon everyone was on board with working differently — the telephone call center, front desk, nurses, providers, medical assistants, clinical care associate, etc.
As a bonus, by changing his schedule to include mini appointments, Douglas was going home earlier each night.
“This is not one guy on a mission,” said Douglas. “I couldn’t have done anything without the ‘yeses’ and the buy-in from our team.”
Find this useful or interesting? We’re constantly sharing stuff like this. Sign up to receive our newsletter to stay in the loop.