What was the problem that needed to be addressed?
Diabetic retinopathy is the most frequent microvascular complication of diabetes and causes approximately 12,000-14,000 new cases of blindness in the U.S. yearly. The Salud Family Health Center (Salud FHC) cares for many diabetic patients with approximately “5,000 patients who have no access to their needed eye care” at all.
What was the innovation?
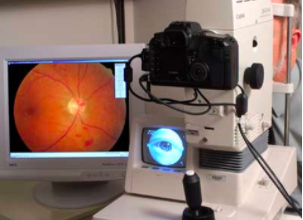
In the original study- the clinic purchased one single-image retinal camera, had staff complete a two-hour training on how to take photographs, had physicians complete a training on how to read the photographs and had a retinal specialist from the University of Colorado re-read all photographs for accuracy.
Today- The multisite FHC has multiple retinal cameras and has a dedicated camera operator in two clinics. In clinics without a dedicated camera operator, the clinics MA’s take the photographs. There are a number of trained physicians that read the retinal photographs at each clinic location site.
Who were the key partners needed?
The Chair of Ophthalmology, a retinal specialist, at the University of Colorado was an integral stakeholder in the process of a successful implementation. He and his group helped train the primary care providers to read the eye photographs and was made available for consultation when needed. The physicians and MAs willingness to learn a new skill was also imperative for successful implementation. Good collaboration and communication from staff, physicians, FHC leadership, and retinal specialists were integral parts of the process.
How was the innovation funded?
Originally, the Salud FHC received a grant from the American Association of Diabetes to determine whether primary care clinics can take retinal photographs themselves, accurately read the photos and to conclude the best access model for in-house diabetic retinopathy screening.
Today, the clinics charge a flat fee of $5 to patients without insurance to cover the visit. They absorb the extra costs of funding the cameras, training or consultation.
What were the results?
The results of the original study showed that 90% of the times, the primary care provider’s readings were completely accurate. The other 10% of readings were mostly due to inadequate photographs with a few abnormalities that needed referrals. To address this issue, more abnormalities were added to the training regimen following the original study.
After diabetic retinopathy screening became an in-house screening, their Health Employer Data Information Set (HEDIS) showed that 80-90% of patients were getting screened in their clinic, in comparison to the approximately 10%-20% of patients in the rest of the country.
What lessons were learned?
Although Salud FHC found that training was simple, they also acknowledged that perpetual practice and full initial camera training was essential to the entire process. Salud FHC recommends that clinics take time to train camera operators well and ensure that the physicians are comfortable reading the photographs.
The clinic recommends that other clinics that replicate this approach create strong affiliations with local ophthalmologists and optometrists to help provide consultation and referral for patients that are determined to need follow-up. It is important for all groups to understand that they are not trying to substitute a full eye exam from a trained ophthalmologist exam, but are aiming to provide accessible diabetic retinopathy screening for those patients that otherwise would not receive screening.
Additional Resources:
Webinar
Dr.Veena Channamsetty from Community Health Center, Inc. and Dr. Tillman Farley from Salud Family Health Centers share how they’ve integrated digital retinopathy screenings into primary care at their organizations.