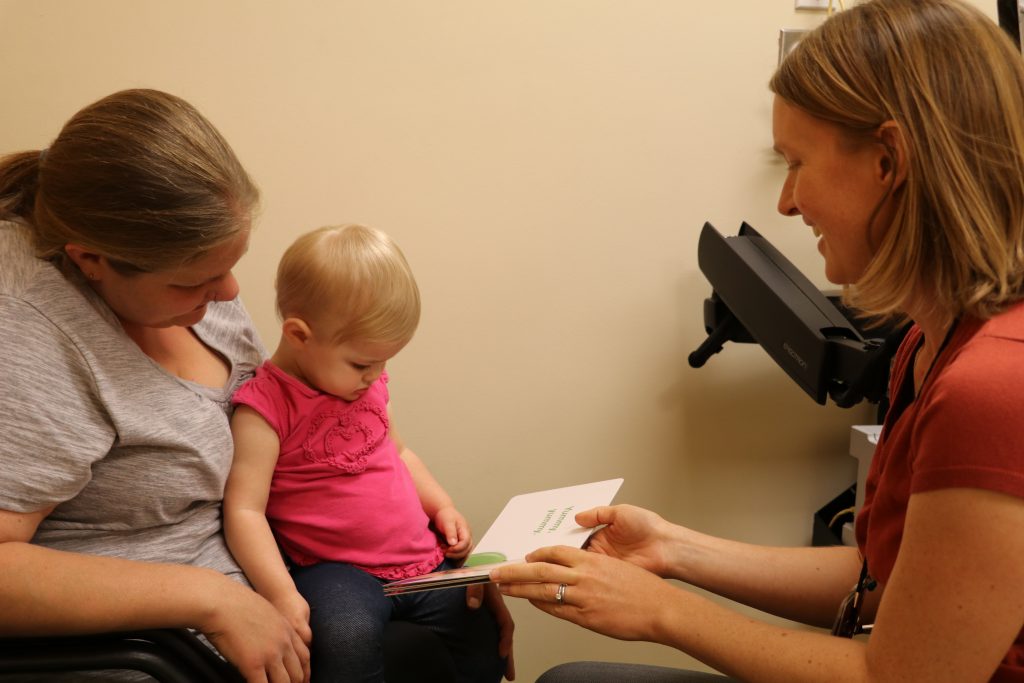
Key Challenges
Manual data entry and missed at-risk patients
Q: What was the problem your organization was grappling with?
A: Previously, Petaluma Health Center was only conducting developmental surveillance, not standard screening. Surveillance is a blunt tool and will miss early signs that a child may have a developmental delay. When delays are identified late, it can become more difficult to get services and services are sometimes less effective. When we looked at our data compared to the prevalence rate of developmental delay, we could see that we weren’t doing a good job identifying kids who needed help. At the same time, we knew that reliably administering and data-entering a three to five page paper questionnaire would be difficult to impossible for our staff to do without some significant changes in their duty assignments. At the same time, we had been experimenting with various kiosk solutions for questionnaires, which met some resistance. We were hopeful that there was a technology solution that would be acceptable to patients, improve the efficiency of assessment, and improve the quality of care.
Q: How did you learn it was a problem? And why was it important to address?
A: Petaluma Health Center hired a part-time pediatrician for consultations around the same time that Redwood Community Health Coalition started to work on regional developmental screenings and referrals. When we measured our baseline referral rate, it was only 10 percent. In order to identify the expected 15 to 18 percent of children with developmental delays — the overall prevalence of developmental delay in a typical community health center population — you have to refer 20 to 25 percent of children for further evaluation. Identifying children with developmental delays and getting them early intervention is a key to long term success in life and learning. We wanted to do a better job of identifying kids who would benefit from early intervention services and get them into care.
Testing
Transitioning from surveillance to a digital, standardized survey tool

Q: Why did you decide to test CHADIS?
A: We were introduced to CHADIS at an eClinicalWorks (eCW) conference. One of the main reasons Petaluma Health Center decided to go with CHADIS is the promise of eCW electronic health record integration that is still in progress according to the vendor — and we’re still hanging on. It is pretty comprehensive in terms of what is offered, if you wanted to expand to other screening tools. Currently, we’re not using it for other screening tools because it’s not an integrated solution yet. However, our medical leadership is still supportive of testing the solution and feels the issue of improving developmental screening and quality of pediatric care is important.
After we started testing CHADIS, we did look into a similar product, Baby Noggin, but there was no eCW integration on the horizon at all. So it didn’t make sense to change or consider it.
Q: Tells us about your pilot.
A: Petaluma Health Center started our pilot with a part-time pediatrician because he was very passionate about the solution and he was already seeing pediatric patients consistently all day and every day. Therefore, we felt like he was a good fit to get the volume we were looking for and to be able to assess what worked and what didn’t.
One of the things that we learned from the pilot was around the timing and workflow of the electronic surveys. When parents received the survey when they were in the back office with the medical assistant (MA), often they wouldn’t finish it before the provider was ready to see their child in the exam room. Ideally, the provider would want to see the results before they do the rest of the assessment, since it would inform next steps for their patient’s care.
As a result, we modified the workflow. We began huddling about our patients in the morning and identifying which children were due for CHADIS. Then we made a note on those appointments, so that when parents arrived and checked in at the front desk, the front desk would give them an iPad to start the survey right away. That made it more likely that the survey would be completed by the time the provider was ready to see the patient.
We also experimented with how much information we would cut and paste into eCW. Initially, we were just inputting the survey result (pass/fail), but the providers wanted to see what questions had negative responses, if any, so they could follow up in a more meaningful way. As a result, we adjusted so that the MA cut and pasted the entirety of the response into the eCW notes.
From the initial pilot, we spread it to the rest of the team working with the pediatrician — a team of four full-time providers and MAs — and then rolled it out at our site at Rohnert Park. When we saw that it was working, so we decided to get more equipment and train another site. We expanded from there.
Our goal when we started was to screen at least 50 percent of our patients between 9-30 months of age who had been seen in the last year. In 2016, we were at 1 percent. We increased to 59 percent in 2018.
Q: How does CHADIS work today in your organization?
A: This is how we use CHADIS at Petaluma Health Center:
- For pediatric patients ages 9-30 months, the goal screen them three times with the Ages and Stages Questionnaire tool (ASQ3) — at 9-15 months, 16-22 months, and 23-30 months.
- Care teams huddle on those patients and patient schedules at beginning of our shift. If pediatric patients haven’t completed a CHADIS questionnaire within the time period, then we’re alerted in our huddle — via data analytics and structured data field in eCW — then we make a note in the appointment.
- When that patient checks in, the front desk gives the parent an iPad, and gets them set up with the questionnaire.
- When the survey is completed, the MA in the back office takes the responses from CHADIS, log in to the web-based platform, finds the patient’s information, and cut and pastes survey responses into eCW.
- The provider reviews it in eCW, then reviews it with the parents in the exam room and verifies any abnormal findings.
- As appropriate, the provider makes a referral to special services for pediatric development.
We’ve also been trying to experiment with ways to get parents to log in and complete the CHADIS questionnaire before they come to their appointment, so they do not have to spend time completing it in the office. The length of survey is approximately 15 minutes. We have not yet been successful with that, but it’s something that we keep intermittently putting more and less energy around.
Lessons & Next Steps
Optimizing clinical decision support, electronic health record integration, and parent engagement outside of the office visit
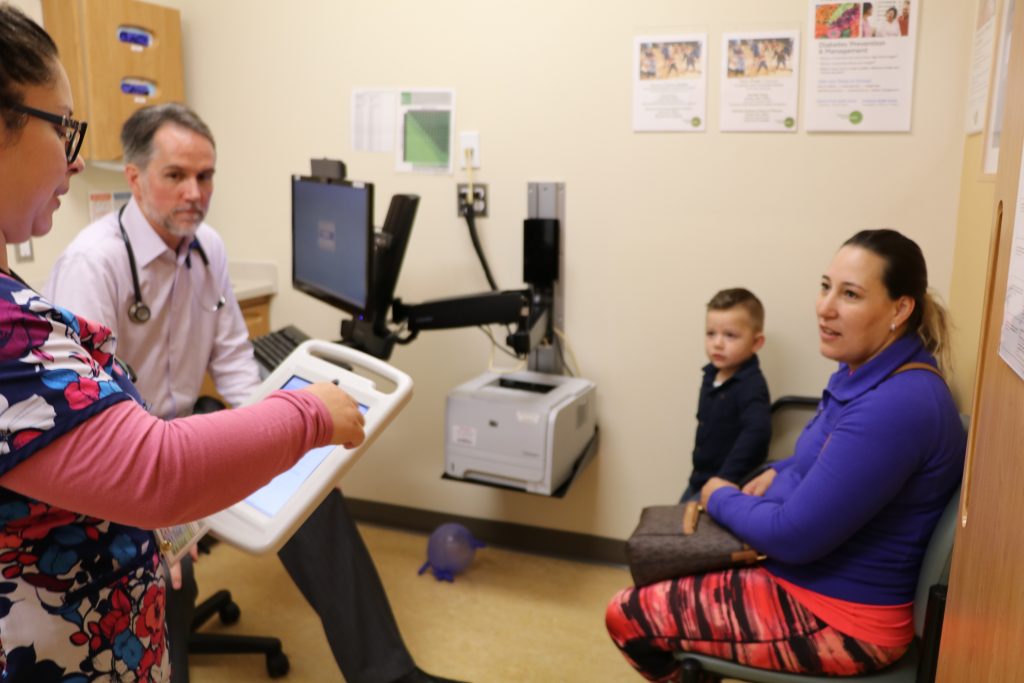
Q: What are some of the key insights from your experience implementing CHADIS?
A: Having identified clinical decision support — or “care gaps” — to help drive who is getting this screening is helpful. It was overwhelming initially for providers to think that every single child that comes in has to do this screening. But over time, as we’ve done more screening, most of those children who come in have already been screened. There’s a little bit of pain in the beginning when you’re starting something new.
We surveyed some parents early on and got really positive feedback on the whole. They felt like the questions were thorough. That questionnaire paired with the interpretation from provider helped parents better understand their child’s developmental progress. We did get some feedback that doing the survey with their toddler in the room was a bit challenging, so we’ve been trying to figure out a way to get them to complete it outside of the visit. Still over half of parents would rather just complete the survey in the office. There’s isn’t one way that is going to work for everybody, so we need to set up different methods that meet people’s needs and preferences.
If we had to do this pilot all over again, maybe might have tested CHADIS with one family practice provider after the one pediatric provider — somebody whose workflows and expectations were more aligned with the overall provider group.
Q: What is next for your team?
A: Petaluma Health Center upgraded its eCW version in September. And at the recent eCW conference, we learned CHADIS integration is still on the work plan, but eCW doesn’t have a definite date for release. We may start using the tool for other surveys, including PRAPARE and the Vanderbilt ADHD screening that we’re currently doing on paper.