To improve access to care, safety net organizations need to get the most out of every day—and out of every member of their team. In the current managed care environment, however, the most efficient ways of handling routine care aren’t always billable. To allow nurses to play a bigger role in care and see more patients in a financially sustainable way, Clinica Family Health Services in Colorado has innovated a tightly timed patient hand-off called a “flip visit.”

Seeing the Problem
When a community clinic doesn’t have time to see a patient, that is care that isn’t being delivered—patients often don’t have any other options they can afford. Providers work frantically to see as many patients as possible, a taxing life. To better use scarce resources to increase access, many clinics seek to give more responsibility to nurses and medical assistants. These staff are often enthusiastic about playing a bigger role in care. But under the rules that govern Federally Qualified Health Centers, clinics are not always allowed to bill Medicaid for nurse’s visits, disincentivizing the practice.
The Patient Perspective
- When you are ill and need care, few things are more frustrating than hearing that you will need to wait to see a doctor. Delays of a day or more can force patients to take more time off work or bend their schedule in costly ways. For patients tight on time and pressed by distressing conditions, not being able to see their primary care provider can drive them to opt for an expensive or unnecessary ER visit instead. For others it can mean foregoing care altogether.
- Same-day access to care also increases patients’ sense that taking care of their health is easy and convenient.
- For routine illnesses, the difference between seeing an MD and an experienced nurse is marginal if the treatment is the same.
The Provider Perspective
- At busy safety net clinics, doctors often spend their day rushing from one 30-minute appointment to another with little downtime to catch up on charting or other work. The flip-visit workflow gives doctors sometimes ten minutes each hour to see to this work, allowing them to leave the workday with less to do later.
- Diagnosing and treating common minor illnesses—sore throats, colds, sinus infections—is relatively standardized and rote. Organizations usually have written procedures for administering this routine care, allowing non-providers such as nurses or medical assistants to deliver the same treatment a physician would.
- Nurses in primary care clinics spend much of their time doing telephone triage. Flip visits get nurses off the phone and seeing patients, which gives them valuable experience and improves job satisfaction.
Best Uses, Biggest Impacts
Flip visits work best for patients coming in with minor acute illness or requiring relatively routine care for non-chronic conditions. Sore throat, fever, headache, rash, pink eye, cold symptoms, lice or scabies, urinary tract infections, and ear pain can all likely be treated based on established protocols. Nurses can also handle routine needs such as medication refills, prescribing birth control (or emergency contraception), removing casts or sutures, administering injections, checking blood pressure or baby weight, and performing ER or wound care follow-up. By using flip-visits for these cases, it serves the dual purpose of easing provider schedules and giving nurses the chance to work more closely with patients and gain experience.
How It Works
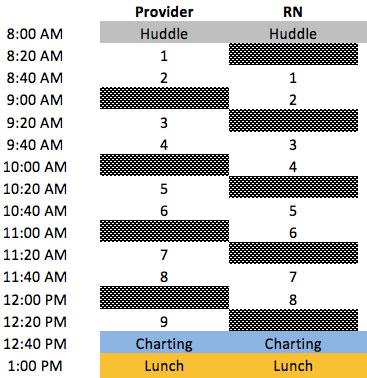
- In a “flip visit,” a nurse or other assistant provider does the bulk of the work on a visit and then hands the patient off to a provider, who briefly checks and adjusts the nurse’s diagnosis and care plan. This converts the nurse’s visit into a billable provider visit
- A provider doing flip-visits should schedule their day in hour-long cycles: two standard twenty-minute visits, followed by a twenty-minute segment devoted to charting and paperwork and picking up the “hand-off” of a flip visit.
- When a patient calls in seeking care for minor acute illness on a day with a full schedule, the staffer taking the call explains that their providers are booked but offers the patient a same-day nurse’s visit instead. A standard script could go something like this: “We can get you in today with a nurse who will assess your concern, and we will do our best to have a provider see you as well.”
- When the patient arrives for their appointment, a nurse takes their patient history, does a physical exam, and works up tests. This is timed so that the end of the visit takes place during the downtime/flip visit part of the provider’s schedule.
- In the last minutes of the visit, the nurse confers with the provider. Nurses should be trained to present the case with the patient’s name, age, pertinent medical history, both symptoms and negatives, and how the patient appears on the physical exam.
- The provider checks and expands the nurse’s physical exam, discusses the case with the nurse, and together they decide on an assessment and care plan. The provider also prescribes medications if needed.
- The nurse explains the assessment and care plan to the patient, goes over warning signs and follow-up, and does any basic education the case requires.
- Providers on a full flip visit schedule can typically do 4-5 flip visits each day, each one requiring only five to eight minutes of the provider’s time and twenty to thirty minutes from the nurse.
Lessons from Practice
- Clinica found that flip visits required a whole new level of communication within care teams. Nurses and providers are now talking in a much more detailed way about individual patients. This requires creative adjustments to workspace to accommodate this communication and the precise timing the handoff requires.
- To increase staff enthusiasm for the flip visit program, Clinica created badges and materials with the slogan “Ninja Nurses FLIP IT!”
What’s Next?
The flip visit pilot program at Clinica was part of a larger plan to expand primary care access by ten percent by the end of 2015 without adding any providers. Feedback on the program from providers, nurses and patients was overwhelmingly positive. With the pilot ending, Clinica plans to continue the flip visit workflow at a lower level, but hopes to be able to expand the model to more care teams in the future.
Learn More
- Clinica Family Health Services is a safety net organization providing primary care near Boulder, Colorado. Visit their website: clinica.org
- Clinica presented on their innovative flip visit workflow at the spring 2014 meeting of the Safety Net Innovation Network.
- Download a PDF version here.
Find this useful or interesting? We’re constantly sharing stuff like this. Sign up to receive our newsletter to stay in the loop.


