What is the best way to convince people in our country to get vaccinated?
One sure-fire way NOT to do so: Argue with a COVID vaccine skeptic until you are both worn out. Instead, tailor the solution to patients’ views on vaccination and the barriers they face.
That was part of what participants learned in “COVID-19 Vaccine Personas,” a webinar co-sponsored by CCI and the National Association of Community Health Centers (NACHC) that featured research from Surgo Ventures and stories from front-line providers.
WHO SHOULD READ THIS ARTICLE And Watch the Video?
Anyone interested in learning more about the five COVID-19 Vaccine Personas and how to engage them.
Download Surgo Ventures slides
More resources are available at the end of this article
Why are some people avoiding vaccination?
“Discussions about demographics and vaccination rates have been very helpful, but they’re not very actionable,” explained Dr. Sema K. Sgaier, co-founder and CEO of Surgo Ventures and adjunct assistant professor at Harvard T.H. Chan School of Public Health. “I think what we really need to understand are those underlying reasons that people are not getting vaccinated, which are very genuine, and how we target the right solutions to the right people.”
To figure out the reasons Americans were shying away from COVID vaccinations, Surgo Ventures conducted a national survey of U.S. adults that revealed the top barriers to vaccination in all 50 states. (See a state-by-state breakdown here.) The organization then used a “precision health approach” to group people into five distinct profiles, or “Vaccine Personas,” based on their barriers to vaccination and the way they viewed the vaccine.

Setting aside the profile called “The Enthusiasts” (40% of the population), who were uniformly eager to get vaccinated, Surgo Ventures has urged U.S. health care officials and providers to focus on the group of Americans their research found “persuadable” (43% of the population).
“What’s especially tricky about COVID-19 is that unlike a ‘normal’ vaccination campaign, we have extremely limited time, so we can’t waste trying to convince people who simply won’t be convinced,” said Sgaier.
“The approach we took is what we call psycho-behavioral segmentation, which is an approach that’s widely used in marketing. It’s really about bucketing people to different groups based on the ways they relate to a product or a service,” Sgaier said. This, she said, allows health officials to target their strategies in ways that bypass demographic categories like age and race – especially useful since all five groups include a mix of different ages, races, and political affiliations.
No “one size fits all” solutions
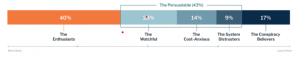
The group used this approach to identify five distinct “vaccine personas” in the United States: the Enthusiasts, the Watchful, the Cost-Anxious, the System Distrusters and the Covid Skeptics (The Conspiracy Believers).
“Once we understand the profiles that people are a part of, we can actually think of very targeted solutions,” said Sgaier. “You may ask, ‘Okay, how do I know what typology a person is that I meet, or a person in my family? Well, you can ask six simple questions, which we were able to develop, which take less than a minute. And with 97% accuracy, the answer to these questions will tell you whether a person is a skeptic, costs-anxious or watchful, and so on, and that will enable you to actually tailor the response.”
“It is really important to listen and acknowledge and not to be confrontational, and then to continue the conversation,” Sgaier added. “So it is really about listening and acknowledging and providing facts rather than combating their facts.”
Here are some findings and recommendations from Surgo Ventures and other panelists about how to reach people who belong to the four profiles, or vaccine personas, who are holding down our vaccination rates.
The ‘Watchful’ (20% of the U.S. population)
States most affected include Delaware, Hawaii, and Rhode Island
Social norms count here. “Before they get the shot themselves, people in this segment first need to see that others in their peer group or community are getting vaccinated and having safe, positive experiences,” reports Surgo Ventures.
For this group, being able to ask questions is important, according to Shelley Spires of the Albany Area Primary Health Care, a safety net health center in South Georgia. “A lot of people in our own health care workforce were initially hesitant to get the vaccine,” said Spires, noting that 117 of the health centers’ 371 employees developed COVID-19 in the first three months of the outbreak.
After the center convened “three wise women” – including a former NIH employee – to explain how the vaccines were made and to talk about safety, vaccination rates rose from 30% to 50%.
How's the #COVIDvaccine rollout is going for Albany Area Primary Health Care in Georgia? Hear that and the latest ACIP updates in the final "Ask Me Anything" in our series. Watch the recording over your lunch break: https://t.co/1HuhNeH9AH pic.twitter.com/XfeUTDHgxT
— NACHC (@NACHC) February 8, 2021
The ‘System Distrusters’ (9% of the population)
States/areas most heavily affected include Washington, D.C., and Maryland
This group is composed largely of populations that have historically had experiences with medical racism in the U.S. health system, a group that includes many Blacks, immigrants, and refugees. Spires reports that her health center has tailored different messages for various groups, including high schools and a consortium of black pastors that providers meet with regularly. “The message is the same, but it may be expressed a little differently so it resonates with a particular population,” she says.
Surgo Ventures also suggests hosting vaccinating in trusted settings outside the healthcare field that reflect the community; being transparent about equity; and having listening sessions with local community leaders after asking “What is your ideal vaccination/health care experience?”
The ‘Cost Anxious’ (14% of the population)
States most heavily affected include Mississippi and Alaska
Since time and cost are the primary barriers, Surgo Ventures recommends reminding everyone that the vaccines are free and/or covered by insurance. Based on the high number of “cost anxious” people in Mississippi and Alaska, for example, the organization recommended focusing on cost there and urging employees to let employees take time off to get the vaccine.
Making it simple for people to get the vaccination is also effective. Deliana Garcia, MA, of the Migrant Clinicians Network reported that her organization offered the COVID-19 vaccine to refugees who were getting out of immigration shelters. “What I see is enthusiasm because many of them have been in detention and they do feel like they’ve been exposed and that there have been no protections for them. So the first opportunity that they’ve had to be vaccinated, they’re really very excited and very willing.”
Young men in detention were more resistant, she added, in part because many reported a fear of needles and others felt it was unnecessary “because they weren’t sick,” confusing the preventive vaccine with a curative injection. “I do believe we’ve not done a good job describing prevention and talking about what it is that you achieve with vaccination,” she said. “That kind of education needs to be thought through more carefully.”
It can be a challenge to select just five pieces to highlight each week. Here are some of the articles that we bet you haven’t seen yet. #FiveOnFriday
— Migrant Clinicians Network (@tweetMCN) May 28, 2021
Despite this, there were some significant achievements, said Garcia, who was talking from her parked car in rural Texas on a trip visiting immigration centers on the US Mexico border. U.S. medical school personnel, she said, had been able to reach maquiladora owners in Tijuana and get permission for workers to cross the bridge to San Diego “where they were met by U.S. nurses and received county vaccines,” said Garcia. “Of the 10,000 doses distributed, 9,000 went to maquiladora workers and 1,000 went to immigration personnel on the Mexican side because they had not yet been vaccinated. And these are individuals who move back and forth – they work in Tijuana and live in San Diego.”
Most COVID Skeptics “not open to persuasion in the short-term”
There are also the ‘COVID skeptics,’ (17% of the population), who are concentrated most heavily in the states of Arkansas, North Dakota, and Nevada. All Covid Skeptics believe in at least one conspiracy theory about the vaccines: 84% think the government is exploiting COVID-19 to control people; 65% think the disease was caused by “a ring of people who secretly manipulate world events”; and 36% think microchips are implanted through the COVID-19 vaccine, according to Surgo Ventures’ research. Cautioning that this group may not be open to persuasion in the short-term, Surgo Ventures recommends focusing on the other three groups pushing down vaccination rates.
In her personal experience, Garcia has also found it hard to dissuade migrants convinced by a conspiracy theory.
“I’ve spoken to folks who might not have originally been skeptical, but the amount of negative information that came out in social media, WhatsApp, and Facebook and Twitter, Instagram, all sorts of things was so intense that they then became skeptical of the value of the COVID vaccine,” Garcia said. “We started to see so many messages that [vaccination] was an effort ‘to implant a chip in my arm so that I could be tracked because people wanted to know about my immigration.’ I had a gentleman who had signed up for his vaccination, but between that time and when I saw him, he was bombarded with so much negative information that he was unwilling to consider it again. He said to me, ‘I am really afraid, I’m very afraid of this. I don’t know what it means, but something is going on and it feels like they’re trying to hurt me.’”
On the other hand, she has seen some tremendous successes. “The Hispanic Construction Workers Association called in the foremen to say, bring in your workers. And that it wasn’t obligatory, but as a benefit of membership. And more and more, we started to see construction workers coming in in large numbers to be vaccinated. And that was one of the groups we were working with which was most strongly resistant to the vaccine. They didn’t see the value, it took time, the skepticism, all of that was present. But things really moved in a different direction.”
Resources
| National Association of Community Health Centers | http://bit.ly/CovidResponseCHC
http://bit.ly/COVIDcommstoolkit https://www.healthcenterinfo.org/piority-topics/covid-19/covid-19-vaccine-distribution/ |
| CareMessage COVID-19 Messaging Platform | More information: https://bit.ly/3fiThz6
Email Contact: Jessica Day at [email protected] |
| Local Initiatives Support Coalition (LISC) Vaccine Access Fund | https://www.lisc.org/covid-19/vaccine-access-fund/
Contact: [email protected] |
Find this useful or interesting? We’re constantly sharing stuff like this. Sign up to receive our newsletter to stay in the loop.

