Top Takeaways
|
Whatever catchy acronym you favor—WOWs for Workstations on Wheels or COWs for Carts on Wheels—rolling workstations offer providers a convenient, private space for virtual care. Equally important, it looks like they are here to stay.
This is especially important in clinics where space is at a premium. As the pandemic continues to unfold, it’s clear there are not enough rooms and privacy to meet the demand for virtual care. This hybrid scheduling solution — using portable carts equipped with tablets to conduct visits with remote patients — allows providers to easily toggle between in-person visits and connecting with patients via screen or phone in the same exam room.
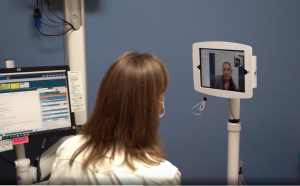
That’s the consensus from two health centers — Neighborhood Health Care and Petaluma Health Center — exploring solutions to deliver high quality, compassionate virtual care that is accessible for all as part of CCI’s Connected Care Accelerator (CCA).
In both cases, the mobile innovations have proven so successful that they’re keepers, a part of everyday practice at both health centers now: Seeing patients both remotely and in person is expected to remain in play in a post-pandemic world. The workstations on wheels didn’t require major workflow changes at either site, and they allow for flexibility in scheduling for patients and providers alike. Here’s a look at how these two health care centers rolled out this innovation.
Neighborhood Health Care
Neighborhood Health Care, a federally qualified health center based in Escondido in Southern California with 19 mostly urban clinic locations, serves 75,000 patients across San Diego and Riverside Counties. Neighborhood Health Care wanted to find a way to make sure providers and patients could access virtual care when they needed to, maintain continuity in health center workflows, and minimize the stress of switching from in-person to virtual modalities.
Clinic leaders pondered three main questions: With the right support, could medical providers and care teams integrate video and phone visits into clinics set up for face-to-face appointments? What equipment would work best? Would continuity be impacted?
After consulting with providers and care teams, Neighborhood came to the conclusion that the best solution for hybrid visits was to duplicate a traditional visit sequence in exam rooms assigned to providers. This required more equipment. Medical assistants began training on virtual meeting technology platforms—in Neighbors’ case, both Doxy.me and Zoom for video and Digium (part of Sangoma) for phone-only connections—to facilitate these visits. Not every patient has access to a tablet, says Jeff Glenn, Neighborhood Health Care’s chief operation officer, and some patients simply prefer phone to video consultations for privacy reasons.
As Maura Mireles, Neighbor’s director of operations, explains in a video of how Neighborhood’s virtual cart visit concept works, medical assistants contact patients and send them a unique link prior to their appointment. They then wheel the carts with a singular tablet device that includes both a camera and microphone into an available exam room. There, they review vitals and field concerns—as they would in a standard visit—before letting primary care physicians know the patient is ready to be seen. This maintains patient privacy and doesn’t require any extra technology set-up on the provider end.
The program, piloted at the health center’s Escondido flagship clinic, has since been rolled out to 17 of the center’s locations; there are now 87 WOWs in use across the organization. There were some connectivity issues early on, since sorted out as platform bandwidth stability has improved with time, says Glenn. The WOWs also required staff buy-in and training for medical assistants and education for patients and providers, but the implementation was pretty straightforward and seamless, notes Glenn, especially with a high-level investment for this alternative shift in healthcare delivery.
Currently, Neighborhood sees 60 percent of its patients in person, 20 percent via video, and 20 percent via phone, says Glenn. In-person visits had climbed back up to 75 percent before the Delta virus variant hit.
“Being able to enter an exam room and find my patient connected via video and ready for the visit allows for better diagnosis and patient outcomes,” says physician Melissa Bishop, who serves as Neighbors virtual care team director. This way the allotted time for a routine visit, notes Glenn, is all devoted to patient care — not connectivity concerns. Watch Neighborhood’s video to see how its providers use the Workstations on Wheels.
Petaluma Health Center
Petaluma Health Center, a federally qualified health center that serves 35,000 rural and suburban residents annually in Sonoma and Marin Counties in Northern California, also wanted to find a way to make sure providers and patients could access virtual care when they needed to, maintain continuity in health center workflows, and minimize any challenges of switching from face-to-face to virtual visits.
At first the staff was skeptical that the center could effectively incorporate video visits into an in-person schedule without significant disruption, according to Jessicca Moore, director of innovations at Petaluma Health Center. After all, there was a learning curve: Medical assistants had to become familiar with the mobile version of Webex, an online video conferencing platform that facilitates virtual meetings, and be able to support patients who hadn’t previously connected with the center in this way. Webex can be accessed via computer, tablet, or mobile phone. But as the health center’s how-to video shows, walking patients through the process proved simple and takes just a few minutes.
As the video explains, Petaluma set up tablets on rolling stands for each care team. Medical assistants “room” patients on video in exam rooms and mark them “ready,” as if they were patients arriving for in-person care and waiting in the waiting room. They remind patients to keep their video on and to unmute themselves for the meeting. The important thing was to ensure that providers didn’t have to negotiate for a video set-up as the patient was due to “arrive,” according to Moore: The virtual exam room had to be ready to roll.
To make this work, the technology innovation team needed to remove any potential technology barriers and make it as much like an in-real-life visit as possible. With this in mind, virtual workflows were adapted to match the face-to-face model: They placed a defined flow for “ready” in the electronic health record, changing the color and adding the room number so the whole team knows when a patient is ready on video and where they are virtually located.
As in real life, providers still go into an exam room with a patient who is ready and waiting to see them. Also, as in real life, sometimes patients must wait to see their provider, so there’s a virtual waiting room. Perhaps mimicking real life, too: People tend to be most on time for video visits scheduled at the beginning or end of the day, notes Moore.
lessons Learned
- Mobile technology increases flexibility and is readily scalable with minimal cost.
- Providers and clinical teams are more effective than the call center at “selling” a video visit to a video-hesitant patient, according to Moore, likely because of their first-person familiarity with the product.
- The virtual carts complement rather than interfere with in-person care, which is gaining traction as more people are vaccinated.
“Using tablets to connect patients to their video visit during in-person visits makes the flow of things go so much smoother,” says Petaluma Health Center medical assistant Vanessa Martin. “The transition from me to the provider is just like it would be for an in-person visit.”
Providers appreciate workstations on wheels, too. “When medical assistants ‘room’ patients with video visits on the tablets during my in-person clinic, I can transition seamlessly from in-person to video without any hassle,” says Petaluma Medical Center physician Scott Holmes.
|
The COVID-19 pandemic upended the way California delivers health care. Health care systems completely restructured their services to keep both their patients and employees safe. Federal policymakers acted quickly to expand coverage and payment for virtual care. The California Department of Health Care Services also dismantled previous barriers to telehealth and began requiring Medi-Cal managed care plans to pay providers for telephone and video visits at the same rate as in-person visits. As a result, many California health care providers rapidly pivoted from in-person visits to virtual patient visits. For these organizations, this shift has been transformational, as they’ve adopted new technology, overhauled workflows, and redefined team member roles. The Connected Care Accelerator — a partnership between CCI and the California Health Care Foundation, with additional funding from the Blueshield of California Foundation — selected 40 safety net healthcare centers in California to participate in a 12-month program that provided funding, methods, tools and hands-on technical assistance to enhance virtual care initiatives. In a series of case studies, CCI showcases the most sustainable and impactful solutions and shares advice for fellow safety net clinics who want to integrate similar virtual care strategies. |




