
Alameda Health System’s Resilient Beginnings Network group on a retreat in Redwood Regional Park (Courtesy: AHS)
Pediatrician Sam Singer admits to feeling frustrated caring for a recently arrived undocumented family from Mexico that included five children, among them siblings with significant developmental disabilities and a baby. Singer, who is bilingual in Spanish and works in the pediatric clinic at the newly renamed Wilma Chan Highland Hospital Campus within Alameda Health System (AHS) in Oakland, did his best to provide the quality care the family needed. Still, he found himself irritated with the mother, whom he thought was flaky — sometimes missing appointments or not following up on key matters between visits.
How wrong was he? He found out after a family specialist at the family partnership initiative DULCE learned that the family needed legal help for an asylum case. The family was referred to the East Bay Community Law Center, DULCE’s legal partner, who agreed to represent them. The law center, in turn, referred the family to AHS’s Northern California Human Rights Clinic (HRC) for forensic evaluations, including those by a pediatrician. Singer happens to be the pediatrician at HRC, where he was able to spend more than the typical 15-minute appointment evaluating the family.
“When I was finally able to make the shift from ‘What’s wrong with you?’ to ‘What happened to you?’ I gained so many insights into what this family had been exposed to, including terrible trauma like gang violence and domestic abuse,” he says. “I was able to see this woman was not flaky at all. She had tremendous resilience. She had saved her children’s lives by bringing them to a safer place. She was an incredible advocate for them. She wasn’t disorganized or uncaring; she was trying to do so much to take care of them. It was a heroic effort.”
Clearly, even a veteran pediatric specialist with a deep and abiding interest in serving the needs of some of the most vulnerable among us — namely children needing asylum — can learn a lot about how to best serve such families from the patients themselves. But as Singer will be the first to tell you, it takes time, awareness, and training around trauma-informed care, and an ability to create an environment where a patient feels comfortable sharing their whole self. It also requires genuine, authentic listening. And it takes a village — or, in this case, a multidisciplinary team devoted to trauma-informed care and resilience. Given how taxing caring for traumatized patients can be for staff, it also takes attention to the needs of team members working in this area to avoid stress, attrition, and re-triggering their own trauma.
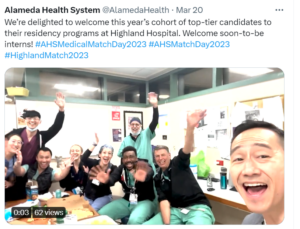
AHS’s Highland Hospital making new members of the hospital team feel welcome (Twitter)
As part of CCI’s Resilient Beginnings Network (RBN), Alameda Health System is strengthening its trauma-informed care at the Highland Pediatric Clinic. From the Oakland-based nonprofit Trauma Transformed, staff have received training in trauma- and resilience-informed systems, known by the acronym TRIS. Trauma- and resilience-informed care emphasizes the importance of understanding a patient’s life experiences and developing a trusting relationship in order to deliver effective care and improve long-term health outcomes.
For children and their families, this safety net clinic is now committed to prioritizing trauma-informed care, a framework based on safety, choice, collaboration, trustworthiness, empowerment, and the knowledge of how both trauma and family strengths can shape people’s lives. That’s vital because childhood trauma, without help from a caring adult or provider, can undermine physical and mental health throughout a child’s life and into adulthood. “It’s a huge thing to have this team,” says Singer, “and to have the chance to sit with and really focus on these issues. This is what drives me in the work I do.”
Tackling trauma
The healthcare providers at Alameda Health System, which serves an economically marginalized and racially, ethnically, and culturally diverse community, are acutely aware of the needs of the people they see. More than 80% of patients bringing newborns to the pediatric clinic have at least one adverse childhood experience (ACE), notes RBN team member pediatrician Robert Savio, former chief of pediatrics at Highland Hospital. More than 43% have four or more ACEs, which is more than twice the state average — and which, without buffering from trusted adults, can significantly raise their risk of developing chronic disease, substance use disorders, and mental ills throughout their lifespan.
As Alameda County’s public health care system, AHS—which includes three acute care hospitals, four ambulatory care wellness centers, four post-acute facilities and the only psychiatric emergency department in the county—strives to eliminate health disparities and barriers to access in the county. Challenges in the region, which includes Oakland, are vast: a growing wealth disparity gap, affordable housing and homelessness, mental health and substance use disorders, and community and family safety.
Screening for ACEs and social needs in pediatric clinical settings promotes early intervention for childhood trauma and can serve as an entry point for safety net clinics committed to providing trauma-informed care. This is especially true when these tools are combined with other efforts to promote resilience with patients and families, such as referrals to sports, peer and friend groups, school and community involvement, and other tools to reduce stress.
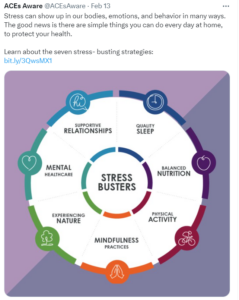
California has helped support ACEs screening and treatment throughout the state (Credit: ACEsAware)
Without support, toxic stress from ACEs – linked to childhood asthma, obesity, behavior and learning problems in childhood and chronic diseases like heart disease and cancer as well as depression and other mental ills in later life — can have a significant effect on patient health. Having an RBN team has been a crucial step for the pediatric clinic: The team has made great progress, though practitioners concede they have a ways to go before they have a well-coordinated effort with significant engagement with patients and families, solid communication between different resource programs, and well-defined intervention strategies.
“The RBN program got us started doing this work,” says AHS nurse Parish Ford, who is a member of the health system’s RBN team. “We weren’t doing this before, and we don’t plan on stopping.”
There is now a commitment from the top down and from the initial patient contact up to address and improve trauma-informed care at the pediatric clinic and beyond. It’s crucial that staff have the training, resources, and vocabulary to navigate this area of care, say Singer and Ford.
That’s where TRIS comes into play. The training is designed specifically for staff in medical clinics and hospitals to understand how trauma and stress, including socio-cultural trauma, impacts developing bodies and brains, communities, and organizations. It also offers strategies for individual and organizational resilience. The goal of this training is to equip a cross-section of the healthcare team to develop shared language and elevate the ideas central to this work, understanding what it means to be a trauma and resilience-informed organization and applying common practices to support well-being.
“Outside of this being great for our clinic, it also makes me look at my own children and try to figure out what I’ve missed…It’s got me more in tune with my kids.”
— AHS nurse Parish Ford on trauma-informed systems training
Part of the RBN TRIS team training consisted of Highland Pediatric Clinic staff having designated time to watch videos on this approach to care and follow up with team-based reflective space to discuss the material. That’s important, because if people aren’t given adequate time to process such information, it’s tough to implement systemic change in the workplace, say the clinic’s RBN team members. In the TRIS training, modules 1 and 2 (Understanding Stress and Trauma; and Reducing Structural Racism and Bias) serve as foundations for understanding the phenomenon. Modules 3 and 4 (Strengthening Resilience and Promoting Safety and Stability; and Cultivating Compassion and Trust and Fostering Collaboration and Agency) are designed to support individual and organizational implementation.
The RBN team were encouraged to see staff paying attention, engaging with each other, making new connections, being respectful, and discussing the topic in a thoughtful and productive way, notes Ford, who found some TRIS content around racial bias triggering. Ford was the only Black employee in the room during one screening. She also raised the importance of figuring out how to incorporate learnings from the sessions into a busy clinic work day—and prompted discussion around the next explicit steps a clinic might take to integrate these valuable insights into practice.
“We want to make sure this training was not a one-off, we’ve got to keep having these conversations and keep [the issue] present, whether it’s about race or any other thing that touches on trauma-informed care,” says Singer, who notes the pediatric RBN team meets once a month.
“When I was finally able to make the shift from ‘What’s wrong with you?’ to ‘What happened to you?’ I gained so many insights into what this family had been exposed to, including terrible trauma like gang violence and domestic abuse. I was able to see this woman was not flaky at all. She had tremendous resilience. She had saved her children’s lives. — Dr. Sam Singer on a refugee patient he was originally frustrated with for sometimes missing appointments
Identifying children and parents who may be dealing with trauma or toxic stress can be difficult for care team providers, especially those that have experienced their own trauma. Health centers now appreciate that providing trauma-informed care and becoming a trauma-informed center cannot only focus on patient care; they must also create a supportive environment for team members. This can include team debriefs; opportunities for reflection, self-care, and work-life balance; and communicating about and providing access to resources to mental health services.
Supporting providers to help patients (and themselves) recover from trauma and devastating loss, navigate difficulties, and rebuild connections is integral to resilience work. Health care workers continue to struggle through the pandemic, experiencing exhaustion, dwindling resources, workforce turnover, and in California, coping with the stress of natural disasters, such as severe drought, wildfires and poor air quality, and recent torrential rains that caused extensive flooding throughout the state.
Trauma-informed care has the potential to be a win-win for both families and staff. “Treating a patient as a whole person helps make them feel more heard; they’ll open up to us, and that helps us help them,” explains Ford, who talks about the ripple effects of this work and its impact on her personal life. “Outside of this being great for our clinic, it also makes me look at my own children and try to figure out what I’ve missed, what I need to do, and what I might need to pay more attention to. It’s got me more in tune with my kids.”
“Just knowing there are so many people who care about this has been inspiring to me,” she adds.
Forging bonds – and having some fun
The pediatric clinic wanted to do something concrete to show support for its hardworking staff, while also prioritizing staff wellness and resilience. The clinic’s RBN team decided to host a wellness retreat at nearby Redwood Regional Park, a sanctuary of towering trees that feels far removed from the frenetic pace of an urban medical clinic. Invites went out to all pediatric clinic staff, who were encouraged to bring spouses, partners, children, and dogs to the offsite meetup.
On a Saturday in June 2022 about 50 staffers and their loved ones gathered for a morning hike followed by a picnic. Barbecue, courtesy of a local caterer, was on the menu. There was no overriding goal other than to hang out together somewhere restorative. There was no agenda and definitely no mandate to talk shop. The name of the game: spending time together in nature for some fun in the sun. Ford delighted in putting together wellness gift bags for participants, as a gentle, welcome reminder about the importance of self-care. She included fortune cookies with inspirational messages, bracelets with words of encouragement, and cards with mindfulness prompts, along with a sweet treat or two. Bretsy Valadez, a medical assistant at the clinic and an RBN team member, spent time decorating the picnic spot in a lowkey yet festive fashion.
The wellness retreat received a resounding two thumbs up from RBN team members and clinic staffers alike. It helped deepen connections among coworkers and forge new ones. Folks felt a little more comfortable with each other, say participants, and many staffers asked when the next retreat was going to be held—a sure sign of success.
Importantly, so that everybody had the chance to attend, Saturday morning clinic was canceled—with the full blessing of leadership—to honor frontline workers in this way. Many people came on their day off, which is a big ask, notes Singer, who also points to how valuable such an event can be for camaraderie. It was an opportunity, says Ford, to get closer to co-workers—without being pulled in multiple directions like they are at clinic. “This kind of activity is good at any time to foster strong interpersonal relationships,” says Singer. “But it was especially good to do on the heels of the pandemic. We got to see each other without masks, without socially distancing, and without the stress of the clinic setting.”
Beyond screening
Like many clinics in California, AHS’s pediatric team is now screening for ACES among its patients. The clinic conducts screenings routinely in English and Spanish, as well as Dari (the Afghan dialect of Farsi), Arabic, Chinese, and Vietnamese using a tool called the Pediatrics Adverse Childhood Experiences (ACES) and Related Life Events Screener, known by the acronym PEARLS. This questionnaire can help determine which patients have experienced stress and/or trauma and could benefit from assistance addressing such concerns. The clinic started a pilot program screening 3- to 5-year old patients; it has expanded its reach to the point that it fairly routinely screens 3- to 11-year-olds. “The goal is universal screening, but there are lots of things that prevent this,” says Singer.
Adding another screening tool into an already packed 15-minute well-child or sick child visit might not sound like much. In fact, it’s a lot. “We know it’s incredibly important and it’s incredibly time-consuming,” says Singer, of feedback from team members who do this work, including nurses, medical assistants, and other support staff. “There’s always extra stuff going on any given day at clinic, and just with the regular flow of clinic, [screening] is the most important stuff we do,” says Singer. He adds that it is also “emotionally taxing,” noting that the clinic’s nursing and support staff are most impacted. “You’ve got to give respectful space and quiet around something so heavy,” he says. “There’s a push-pull because we’re all harried, we’re all running a little late but you want to be able to ask about things that can affect emotional and spiritual health.”

The team is cognizant of making sure to follow up on patients who screen positive for ACEs. Children under 5 are typically referred to Alameda County’s Help Me Grow program, which has funding and data tracking support, and offers resources and services to ensure that young children reach their optimal development. For older children, the clinic offers more behavioral health support. The team would like to do more data gathering for this age group. The clinic also distributes books to families—in several languages—that focus on stories around resilience. As the RBN team sees it, they’re engaged in a three-pronged approach: TRIS training, ACEs screening, and patient intervention, which they haven’t spent as much time and resources on as yet. But they see it as a vital next step to their RBN work.
While behavioral health referrals are crucial for many ACEs- positive patients, Singer says he’d also like to see other kinds of interventions for patients in the mild-to-moderate range of need. “These children may not need a therapist, but maybe there is something else we can do for them. Can we help get them on a soccer team, get them in a church group, have them go hiking?” he asks. “These interventions are not as intensive and don’t require a social worker or a professional to help coordinate, but could also be very helpful.” Singer says he’d also like the clinic to figure out a way to track and gather data on these kinds of “softer” referrals/prescriptions for wellness.
Being part of the RBN team has been a game changer for Singer, who sees the pediatric unit as trailblazers for this work within his organization. He hopes that the RBN message spreads to other areas, including adult care. “This is always with me, I’m always thinking about it. But we don’t always get to talk about it, and we don’t get to make it explicit and share. Having an interdisciplinary team makes a difference; it’s not just doctors talking to doctors, and to me that’s a huge thing,” he adds. “It’s great to have the time and space to think about it. Moving forward, I’m ready for more practical things that we can actually implement.”
Up next for the team to tackle: What does a comprehensive intervention program for resilience and trauma-informed care actually look like in a clinic such as Highland Pediatric? Stay tuned.
Lessons Learned
Make TRIS interactive. Keep staff engaged in the learning process by encouraging participation such as role-playing exercises and break-out groups.
Center patient experiences. Children and their parents and caregivers are more likely to share about traumatic or stressful experiences if they feel they are in a safe environment with someone they feel comfortable with and trust. Building such relationships takes time and patience.
Schedule time for staff reflection. Change happens when there is space to talk about the challenging and often disturbing revelations team members confront.
Prioritize staff wellness. Schedule downtime away from the clinic or hospital and make it a mission to have no agenda beyond rest, relaxation, and socializing.
Protect team time. Make sure management prioritizes this work by securing clinic coverage for regularly scheduled team meeting times and other “thought” work in this area.
Alameda Health Services is part of the Resilient Beginnings Network, a learning program that promotes trauma- and resilience-informed care so that 100,000 young children and their caregivers in the San Francisco Bay Area have the support they need to be well and thrive. The Resilient Beginnings Network is powered by the Center for Care Innovations, an Oakland-based nonprofit that promotes health equity and innovation in the health care safety net, and by Genentech Charitable Giving.
Find this useful or interesting? We’re constantly sharing stuff like this. Sign up to receive our newsletter to stay in the loop.

